 |
 |
- Search
| Arch Hand Microsurg > Volume 28(3); 2023 > Article |
|
Abstract
Post-burn scar contracture associated with deep second-degree or higher burns in the joint area can lead to joint immobility and may cause chronic ulcers, substantially impacting patients’ quality of life. Surgical intervention is necessary, with local flaps or skin grafts being the first option. In extreme cases, free flap transfer may be required to address large defects that occur after contracture release. This study presents a successful case of reconstruction using free flap transfer in a patient with severe post-burn scar contracture, which resulted in a club-like deformed ankle with a nonfunctional joint. Despite the extreme deformity and nonfunctioning joint, we utilized a thoracodorsal artery perforator flap to stably cover the newly fused joint in a neutral position. After reconstruction, the patient was able to wear shoes and ambulate. This case highlights the potential of free flap transfer even in the most challenging situations where joint function is severely compromised.
Post-burn scar contractures associated with deep second-degree or higher burns in the joint area may not only lead to soft tissue complications but also significantly limit joint mobility, consequently causing substantial restrictions in daily activities. The knee, ankle, and metatarsophalangeal joints are the most commonly affected sites in the lower limbs [1]. Among these affected sites, when contractures occur in the ankle and foot, they not only limit the range of motion but also make it challenging to wear shoes and impair ambulation. Impaired walking and difficulty wearing shoes can contribute to the formation of ulcers, potentially leading to undesired chronic ulcers and substantially impacting the quality of life. Since contractures often accompany physical pain and emotional distress, appropriate and timely surgical intervention is necessary [2].
Previous studies have shown that surgical release of joint scar contractures significantly enhances patients’ quality of life [3]. If contracture release can be achieved through local flaps or skin grafting, it is the most favorable option in terms of surgical time, hospitalization, and recovery period. However, if the contracture is severe and cannot be addressed by such flaps, free flap transfer should be considered [4]. In such extreme cases, the required soft tissues are deep and extensive due to the degree of contracture. This study aims to present a successful case of reconstructing an extreme post-burn scar contracture, which led to total fusion of the ankle joint in a hyper-dorsiflexion state.
This case study received research approval from the Institutional Review Board of Hanyang University (No. 2023-07-004). Written informed consent was obtained from the patient for the publication of this report, including all clinical images.
A 58-year-old male patient suffered a third-degree burn on his right foot due to a burn incident that occurred before the age of one. The right ankle developed band contracture in a hyper-dorsiflexed state, which over time led to a club-like fusion. Ankle motion was entirely impossible. For ambulation, the patient would bind his foot to a basketball shoe and use crutches for partial mobility. Although the skin was not fibrotic, scars were observed in the calcaneal region due to the recurrent occurrence of ulcers (Fig. 1). However, although it was belated, surgical intervention was attempted to enable at least minimal walking. Arthrodesis in neutral position was planned to disperse weight-bearing pressure and prevent wound recurrence, but surface reconstruction was needed after ankle joint release. A local flap was not suitable due to insufficient soft tissue in the ankle and foot region, and a skin graft was inappropriate for inset on exposed bone and tendon with a high risk of secondary contracture.
Free flap reconstruction was considered necessary. Owing to a 14-year history of diabetes mellitus, mild calcification and occlusion were noted in the vessels of the foot. Nevertheless, sufficient circulation was preserved through the formation of collateral vessels. Fortunately, the anterior tibial artery (ATA), posterior tibial artery (PTA), and peroneal artery at the ankle level, which could be used as recipient’s vessels, were all intact. The diameters of these arteries were 1.74 mm for the ATA, 2.05 mm for the PTA, and 1.44 mm for the peroneal artery (Fig. 2). A thoracodorsal artery perforator flap was chosen due to its flexibility to maintain the neutral position and the need for a thin flap to allow future shoe wear. A flap with a long axis of 20 cm, short axis of 10 cm, and pedicle length of 8 cm was elevated from the right flank donor site in the supine position. After the orthopedic surgery team performed talonavicular joint capsulectomy and arthrodesis in neutral position with a Kirschner wire, thoracodorsal artery and vein were anastomosed to the ATA and vein, respectively, in an end-to-end fashion (Fig. 3). The flap was stable, and the patient was discharged on postoperative day 9. The wire was removed at 5 weeks postoperative, and the weight-bearing ambulation began 3 months after the surgery. Flap debulking procedure was performed at the patient's request 17 months postoperatively, and no complications, including pressure ulcers, were observed during the 18-month follow-up period after the surgery (Fig. 4).
Post-burn scar contracture is a common complication of burns, particularly in deep second-degree or third-degree burns. The pathophysiology of this condition is related to the healing process of burned tissues. Initially, burned tissues undergo an inflammatory response and tissue damage, leading to the formation of granulation tissue. The granulation tissue is then replaced by new collagen and other extracellular matrix components in a process called remodeling. However, in cases of extensive or deep burns, the remodeling process can be disrupted, resulting in the deposition of less elastic and pliable collagen fibers that form a dense and disorganized scar. This contracted scar can limit the mobility and flexibility of the affected area and cause tethering of the skin and underlying tissues due to the scar tissue’s contraction and pulling on healthy tissue. The resulting adhesions and deformities can lead to post-burn scar contracture, which restricts joint mobility and may result in severe functional impairment.
Although attempts have been made to compare different procedures for intervention after a burn occurs, a conclusive and effective conclusion has not been reached [5]. But there is research suggesting that local flaps are superior to full-thickness skin grafts in terms of color and secondary contracture in cases where burn scar contracture falls within the range of possible flap or graft [6]. Generally, when dealing with extensive burns and third-degree burns or higher, well-vascularized and abundant tissue flaps are often necessary. In extreme cases like the one presented in this study, where the concept of contracture release goes beyond simply releasing the contracture and requires the formation of a neutral joint, the use of well-vascularized free tissue to cover exposed bone and joint capsules becomes essential. Even in severe cases of burn scar contracture release, similar considerations would apply.
In this case, a thoracodorsal artery perforator flap (TDAP) was utilized. TDAP has been shown in previous studies that allow for the harvesting of an extensive large flap, provides well-vascularized tissue, ensures long pedicle length, and offers flexibility [4,7]. It is particularly suitable for three-dimensional reconstruction procedures such as joint forming, which may require the use of a chimeric flap [8].
This case study provides insight into an extreme case of post-burn scar contracture and demonstrates how successful reconstruction can be achieved through the use of free flap transfer without any complications. Such experiences and research can provide hope that even in cases of extreme deformity, radical reconstruction attempts can be made to improve the quality of life for patients.
Fig. 1.
58-year-old male patient with hyper-dorsiflexion of the ankle joint and repeated ulceration and healing due to inadequate medical services, resulting in total fusion of the ankle joint, presented to the clinic. Preoperative clinical photograph presenting a frontal view (A), lateral view (B), foot anteroposterior X-ray (C), and foot lateral X-ray (D).
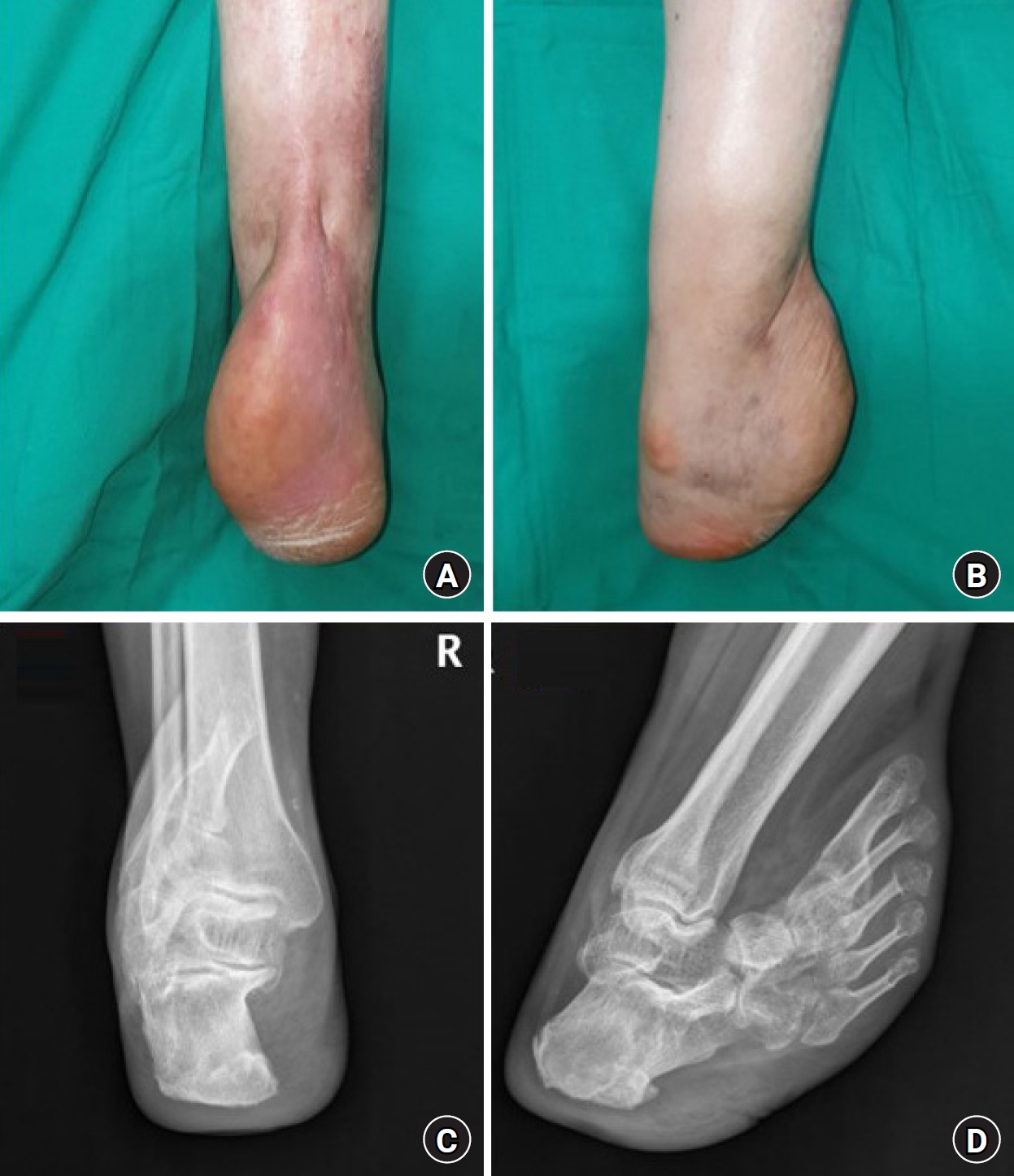
Fig. 2.
Computed tomography angiography revealed preserved patency of the right anterior tibial artery, posterior tibial artery, and peroneal artery at the ankle level (red arrow).
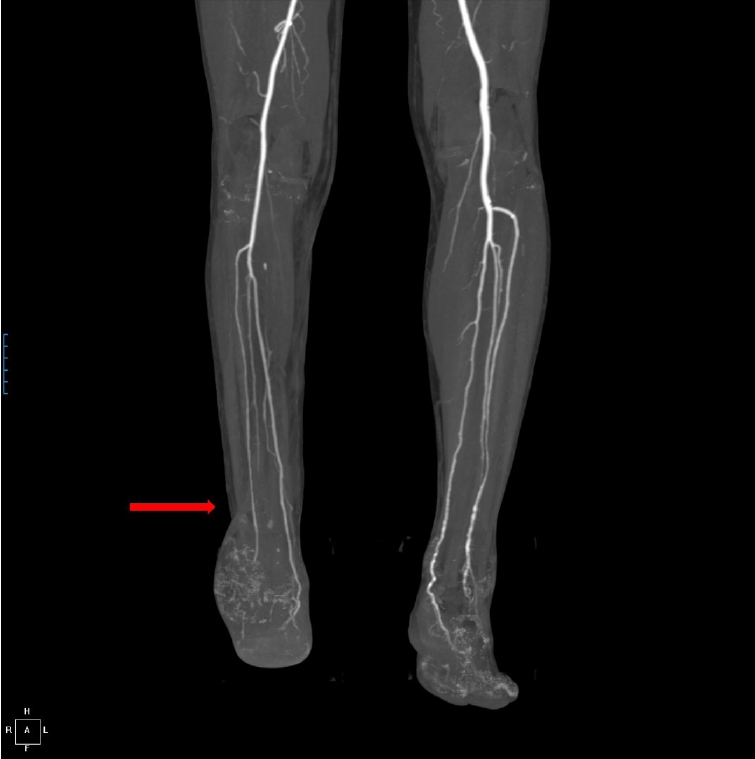
Fig. 3.
(A) An immediate preoperative clinical photograph showed walking impairment and chronic ulceration in the ankle. (B) The orthopedic surgery team performed talonavicular joint capsulectomy and arthrodesis with a Kirschner wire in the neutral position. (C) A thoracodorsal artery perforator flap with a long axis of 20 cm, short axis of 10 cm, and pedicle length of 8 cm was elevated. (D) An immediate postoperative clinical photograph showed a stable ankle joint without any acute complications.

References
1. Mani MM, Chhatre M. Reconstruction of the burned lower extremity. Clin Plast Surg. 1992;19:693-703.


2. Riaz HM, Mehmood Bhatti Z. Quality of life in adults with lower limb burn injury. J Burn Care Res. 2020;41:1212-5.


3. Hendriks TCC, Botman M, de Haas LEM, et al. Burn scar contracture release surgery effectively improves functional range of motion, disability and quality of life: a pre/post cohort study with long-term follow-up in a low- and middle-income country. Burns. 2021;47:1285-94.


4. Chang LS, Kim YH, Kim SW. Reconstruction of burn scar contracture deformity of the extremities using thin thoracodorsal artery perforator free flaps. ANZ J Surg. 2021;91:E578-83.


5. Stekelenburg CM, Marck RE, Tuinebreijer WE, de Vet HC, Ogawa R, van Zuijlen PP. A systematic review on burn scar contracture treatment: searching for evidence. J Burn Care Res. 2015;36:e153-61.


6. Stekelenburg CM, Jaspers ME, Jongen SJ, et al. Perforator-based interposition flaps perform better than full-thickness grafts for the release of burn scar contractures: a multicenter randomized controlled trial. Plast Reconstr Surg. 2017;139:501e-509e.










