 |
 |
- Search
| Arch Hand Microsurg > Volume 28(2); 2023 > Article |
|
Abstract
Purpose
This study compared the surgical outcomes and quality of life of patients who underwent fasciocutaneous and fascial anterolateral thigh (ALT) free flaps for the reconstruction of traumatic soft tissue defects in the foot.
Methods
A single-institution retrospective review of medical data from 2008 to 2021 was conducted on 20 patients who underwent a fasciocutaneous ALT free flap or fascial ALT free flap in the foot. Information was collected on patients’ baseline information, preoperative characteristics, and postoperative courses. Quality of life was measured through the Foot and Ankle Disability Index (FADI) score. A questionnaire survey was administered to evaluate aesthetic satisfaction and subjective improvement of dryness and sensory function at the surgical site.
Results
The mean flap dimensions were 13.96×4.58 cm and 10.75×3.50 cm in the fasciocutaneous and fascial groups, respectively. The overall flap failure and complication rates were higher in the fasciocutaneous group (total necrosis in one case, partial flap loss in two cases, and vascular complications in three cases). While aesthetic satisfaction and functional outcomes (FADI Sports) showed better outcomes in the fascial group, subjective improvement of dryness and sensory recovery showed better results in the fasciocutaneous group.
Conclusion
In comparison to fasciocutaneous flaps, fascial free flaps demonstrated lower rates of wound complications, higher aesthetic satisfaction, and better functional outcomes, but less improvement in dryness and sensory recovery at the flap site. Therefore, the choice of a flap for foot reconstruction should depend on the plastic surgeon’s discretion and a thorough discussion with the patient.
The foot is more commonly and easily exposed to trauma and injury than any other part of the body due to its anatomical location [1]. Many of the injuries to the foot range from minor fractures to major soft tissue defects, often requiring free flap coverage. This poses a significant challenge for reconstructive surgeons as they must consider not only the function of the foot in terms of gait, but also its sensation, aesthetic appearance, and personal satisfaction of the patient.
First introduced by Song et al. [2] in 1984, the anterolateral thigh (ALT) free flap has been widely used as a main reconstructive option in various anatomical regions. Due to its durability and versatility, it can be useful in foot reconstruction [3]. However, its thickness and bulkiness often result in patient dissatisfaction and poor aesthetic appearance, leading to the necessity of a secondary procedure such as flap debulking [4].
Unlike conventional fasciocutaneous ALT free flap where skin, fat, and fascia are all harvested, fascial ALT free flap is elevated without the skin paddle. First described by Smith [5] in 1980, fascial free flap is useful for its thinness and pliability. Only the fat tissue below Scarpa’s fascia with deep fascia are harvested, creating a thin fascial ALT free flap. The advantage of this flap is that it can cover soft tissue with a thin contour, but it also has the disadvantage that a secondary procedure such as skin graft is essential.
The purpose of this study is to analyze our experience with both fasciocutaneous and fascial ALT free flaps in foot reconstruction and compare outcomes related to complications, number of secondary procedures, and functional and aesthetic satisfaction.
Ethics statement: This study was performed in accordance with the Declaration of Helsinki. The need for patient consent was waived owing to the study’s retrospective nature, and the study design was approved by the Institutional Review Board of Gwangmyeong Sungae General Hospital (No. KIRB-2022-N-002).
A single-institutional retrospective review of patient information was performed for all patients who received fasciocutaneous or fascial ALT free flap for soft tissue coverage in the foot defect from July 2008 to May 2021. When determining the surgical method between fasciocutaneous and fascial ALT free flap, the location of the defect size was primarily considered. For the foot dorsum, which has a relatively low weight-bearing burden, is exposed outwardly, and may cause hindrance when putting on and taking off shoes, it was considered to perform a fascial free flap followed by skin graft to obtain optimal thickness. However, if the surgeon judges that skin graft coverage may be difficult due to the large size of the defect before surgery, a fasciocutaneous free flap was performed. Basic patient demographics, donor site morbidities, complications, postoperative outcome, need for secondary procedure, sensory function and aesthetic satisfaction were recorded. Donor site morbidities were evaluated based on whether they were primarily closed or not. Early complications, including total flap loss, partial flap loss, vascular complications, and infections, were also recorded. All patients completed Foot and Ankle Disability Index (FADI) and FADI Sports (FADI-S) questionnaire to evaluate postoperative disability sequelae in daily living. In addition, an independent patient-centric questionnaire was created to investigate dryness and subsequent discomfort at the surgical site (Tables 1, 2). To measure patients’ subjective satisfaction regarding the aesthetic appearance of their feet, a questionnaire focusing on aesthetic outcomes, including contour, shape, and color, was issued to each individual (Table 3). Respondents answered three questions on a scale of 1 to 5 points (1, strongly disagree; 2, disagree; 3, acceptable; 4, agree; and 5, strongly agree). Aforementioned postoperative outcomes were evaluated at a 1-year postoperative point after all additional surgeries were completed.
The operative technique for the ALT free flap had been previously described in other publications [6]. Preoperative marking of the perforator from the lateral circumflex femoral artery was performed by vascular ultrasonography at the department of radiology by a single radiologist to minimize any technical errors. Preoperative ultrasonography was useful as vascular distribution could vary individually. The flap was designed according to the shape and depth of the defect in the foot. The medial skin was incised to the depth of the fascia. During this process, the rectus femoris was identified with caution. Once the fascia was raised from the rectus femoris, careful visualization of the perforator was done. During the process, meticulous bipolar and Bovie cauterization was necessary to prevent damage to other collateral systems and potential hematoma. Once the perforator was identified, the lateral incision continued. The fascia lata and the skin paddle were dissected from the vastus lateralis. The difference between fasciocutaneous and fascial ALT free flap was the plane of the flap elevation. Fasciocutaneous ALT free flap was harvested in all layers, including skin to the muscular fascia, while fascial ALT free flap was elevated from the Scarpa’s fascia to the muscular fascia. All fascial ALT free flaps were then covered by split-thickness skin graft (STSG).
STSG was mainly harvested from the ipsilateral thigh using a dermatome device. Once the graft was fixed with staying sutures, it was covered with a tie-over dressing. The dressing was taken off after 7 days postoperatively. The degree of graft take was measured based on color, capillary refill, and texture.
Statistical significance between continuous variables of two flap types was analyzed by the Mann-Whitney test, while discrete variables were analyzed by the chi-square test. A p-value less than 0.05 was considered statistically significant. Statistical analysis was conducted using IBM SPSS Statistics ver. 26.0 (IBM Corp., Armonk, NY, USA).
There was a total of 14 patients who underwent fasciocutaneous free flap, of which 12 were male and two were female. The mean age was observed to be 48.64 years. The fascial free flap was performed in six cases, all male, and the average age was 42.17 years (Table 4).
Indication for the surgery for all cases was soft tissue defect caused from major trauma to the lower extremity.
The mean dimension of fasciocutaneous ALT free flap was 13.1×7.1 cm (range, 9–18×6–8 cm) and that of fascial ALT free flap was 14.1×7.8 cm (range, 15.5–12.5×5.5–12 cm).
Overall, the survival rate for both groups was recorded at 95.0%. All free flaps from two groups survived except for one fasciocutaneous free flap with total flap loss as postoperative complication. Partial flap loss was observed in two cases from the fasciocutaneous group and in one case from the fascial group. The most common postoperative complication was vascular complication. Three cases were observed in fasciocutaneous free flap and one case was observed in fascial free flap. A total of three cases required secondary debulking procedure for functional and aesthetical improvement (three in fasciocutaneous group and zero in fascial group). Mean number of additional surgeries after free flap was 1.92 in fascicutaneous group and 2.50 in fascial group. Treatment of choice for donor site was primary closure. Eleven out of 14 fasciocutaneous free flap cases (78.6%) showed successful primary closure of donor site while fascial group showed 100% primary closure rate.
No significant statistical correlation was found between the two groups in terms of total flap loss (one in fasciocutaneous and zero in fascial, p=0.08), partial flap loss (two in fasciocutaneous and one in fascial, p=0.1), and donor site primary closure rate (11 in fasciocutaneous and six in fascial, p=0.08). However, vascular compromise (three in fasciocutaneous and one in fascial, p=0.04), number of secondary debulking procedures (three in fasciocutaneous and zero in fascial, p=0.03), and mean number of additional operations (1.92 in fasciocutaneous and 2.50 in fascial, p=0.04) showed a statistically significant correlation between the two groups.
At 1-year postoperative follow-up at outpatient department, all patients who met our inclusion criteria were evaluated with FADI and FADI-S regarding postoperative disability and daily living discomfort. FADI did not show a statistically significant correlation between the two groups (69.6 in fasciocutaneous group and 70.3 in fascial group, p=0.08). However, fascial group showed a better prognosis than that of fasciocutaneous group in FADI-S (14.5 in fasciocutaneous and 20.7 in fascial). A statistically significant correlation of FADI-S was observed between the two groups (p=0.04) (Table 5).
In addition, patients were assessed with subjective sensory recovery in terms of dryness, nociception, coldness, warmth, tactility, and pressure sense at the point of same postoperative follow-up day. Based on the scores collected from the questionnaires, patients complaining of dryness at the surgical site were more frequent in the fascial group, and discomfort caused by this in daily life was also observed more in the fascial group. A statistical difference between the two groups was observed to be significant (p=0.03 and p=0.02). In the questionnaire on sensory recovery after surgery, the fasciocutaneous group showed better results in terms of pain, cold, and warm sensation (p=0.03, p=0.02, and p=0.02, respectively). Fascial group showed better results in terms of tactile and pressure sensation, but they did not show statistical correlation (Table 6).
A 36-year-old male patient was injured in a motor vehicle accident that affected his left foot and lower leg. After serial radical debridement and negative-pressure wound therapy, soft tissue defect healed but remained with exposed extensor tendons on dorsal area. Free flap coverage was required. ALT fascial free flap measuring 7.0×3.0 cm was elevated from ipsilateral thigh. The pedicle from lateral circumflex femoral artery was anastomosed end-to-end to the dorsalis pedis artery and two vena comitans to subcutaneous veins. During free flap insetting, extensor hallucis longus tendon was excised in order to prevent pressure from being loaded to the anastomosed pedicle. After 4 weeks, STSG was applied. There were no operation-related complications observed during the admission period. The patient showed better FADI-S index regarding postoperative prognosis (23; mean value in the study group, 20.7) than other patients. The patient reported discomfort due to the absence of nociception, coldness, and warmth sensation at the operation site. He only showed tactility and pressure sense. Furthermore, the patient reported significant discomfort caused by dryness at the operation site. However, he reported the highest aesthetic satisfaction score of all patients (90.0%) (Fig. 1).
A 68-year-old female patient suffered from severe crushing injury of her right foot from motor vehicle accident. In order to cover the soft tissue defect with exposed extensor tendons on dorsal side, free flap coverage was planned. An ALT fasciocutaneous free flap measuring 11.0×3.0 cm was elevated. The pedicle of the flap was anastomosed end-to-end to dorsalis pedis artery. One vena comitans and one subcutaneous vein of the flap was each anastomosed end-to-end to two different dorsal cutaneous veins. The patient did not require additional operation. The patient did not have discomfort caused by dryness at the operation site. Also, she showed excellent results on sensory recovery in terms of dryness, nociception, coldness, warmth, tactility, and pressure sense. The patient showed better FADI (102; mean value, 69.6) and FADI-S (32; mean value, 14.5). However, her aesthetic satisfaction score was the lowest of all patients (14.7% ) (Fig. 2).
The ALT free flap is a reliable and versatile option for soft tissue defects and has been widely recommended for its durability and reliability [7,8]. However, in distal extremities where thin contour is required, fascial free flap may be a more suitable option. It can overcome disadvantage of conventional fasciocutaneous free flap in which the flap must be elevated in bulky and thick shape [9]. Foot plays significant role in one’s daily life. Therefore, it is essential to require durable soft tissue coverage to prevent complications [10]. Additionally, the recovery of sensation and functional prognosis are also important considerations.
Previous studies have suggested that free flap coverage of soft tissue defects caused by trauma or diabetic ulcer in lower extremities can result in good functional outcomes and increase possibility of independent ambulation for patients [11,12]. In this study, the functional outcome of patients in each of the two flap-type groups was compared using the widely used FADI and FADI-S indices. After analyzing the prognosis between the two groups, FADI-S questionnaires showed better and statistically significant outcomes in fascial group. However, FADI index, which requires more general items, did not show statistical correlation. Thus, the comparative excellence in terms of ambulation and daily living between fascial and fasciocutaneous free flap has not yet been fully verified. Further study on this area seems required.
Free flaps with denervated skin stimulate the cut cutaneous nerves in the recipient area with a strong neurotrophic stimulus. Suturing the flap to the borders of the healthy tissue, where sensation is present, is crucial to achieving optimal nerve regeneration. Although they resist infection and provide excellent shape with low bulk tissue, scars around the borders and fibrosis between the muscle and skin grafts pose a challenge and result in poor outcomes in terms of recovery of sensation [13]. In this study, it was also found that the sensory recovery of the fasciocutaneous free flap was superior to that of the fascial free flap. Therefore, it seems more beneficial to use a debulking procedure after performing a fasciocutaneous free flap in areas of the foot where sensation is important, where there is an expected problem when wearing shoes, or where ambulation will be affected.
According to Lowrey et al. [14], skin sensation plays an important role in kinesthesia at the ankle. Reduced skin sensation of the foot dorsum results in decreased accuracy and increased variability observed in the ankle joint matching task. Kinesthesia in the ankle is significantly influenced by sensory input from the skin. Therefore, in patient groups where kinesthetic sensation is important at the ankle and much ambulation is required, it may be beneficial to consider implementing fasciocutaneous free flap, which has better sensory recovery on the dorsum of the foot.
Although there may be a possible disadvantage that the patient burden may increase when performing the fasciocutaneous free flap due to potential need for debulking procedure, statistical analysis of the number of additional surgeries between two groups shows that the average number of additional surgeries following fascial free flap was higher (2.5 times), which was statistically significant. In the fascial group, additional surgeries were required depending on the success of skin graft taken. If the take was poor, debridement, local flap, or additional STSG were considered, but most procedures were simple and could be performed under local anesthesia. However, some patients may experience stress or burden as a result. Patients who feel burdened by the need for additional surgery should more actively consider performing fasciocutaneous free flap. It is important to properly explain this aspect during presurgery consultations.
Furthermore, in fasciocutaneous group, despite secondary debulking procedures being performed in the group, overall improvement in aesthetic outcome was not significant, and the average satisfaction level was lower compared to the fascial group. One possible reason for this could be that all three cases in which the secondary debulking procedure was performed at the hospital were limited to surgical excision. Previous study has suggested that liposuction is a commonly used debulking procedure, and this technique can result in substantial enhancements in cosmetic results [15]. In our study, if effective methods such as liposuction were also performed together with surgical excision, it is believed that improvements in aesthetic outcomes could have been achieved. Additionally, all patients planned to undergo debulking procedures through consultations with their surgeon during outpatient follow-up, but some patients refused surgery due to personal or insurance issues. If there had been more debulking patients in the fasciocutaneous group, a more accurate analysis could have been possible, and further study is needed in this area.
Vascular complications were measured to be significantly higher in the fasciocutaneous group (three cases) compared to the fascial group (one case). The vascular complications observed in the fasciocutaneous group included two cases of venous insufficiency and one case of arterial insufficiency. Venous congestion was observed immediately after surgery, but this was improved with leech therapy and external drainage without requiring additional surgery or revision process. However, partial flap loss occurred in two cases. In the case of arterial insufficiency, revision surgery was performed but the flap blood flow did not improve, resulting in total flap loss. In the fascial group, one case of arterial insufficiency was observed, and additional revision surgery was performed to improve blood flow, but partial flap loss still occurred. The difference in complication rates and vascular compromise between the two groups is thought to be due to differences in flap size. According to Rhodius et al. [16], a larger flap size requires more metabolic energy and is therefore more vulnerable to vascular problems, which could increase the risk of flap complications. Large flaps are especially prone to issues like distal necrosis or tissue volume loss and atrophy. Lee et al. [17] also showed that larger flaps in lower extremities are associated with higher complication rates. Based on these findings, we suggest that the larger average flap size in the fasciocutaneous group in our study may impair the ability to tolerate vascular compromise due to the greater metabolic demand of larger flaps, thus resulting in higher complication rates including vascular problems than those of fascial group.
ALT free flap is preferred for its favorable donor site and concealable scar. The donor site is closed primarily most of the time [8]. ALT fascial free flap can enhance this advantage. The present study showed that the donor site primary closure rate is relatively higher in the fascial group compared to the fasciocutaneous group. Since fascial free flap is elevated less bulky than the fasciocutaneous free flap is, it makes donor site closure more favorable. Boca et al. [18] reported that when the ratio of ALT flap width-to-thigh circumference was less than 16%, primary closure was achieved. Depending on the size of the defect, on average, the fascial free flap is smaller in weight and size than the fasciocutaneous free flap, so donor closure will be more favorable.
A limitation of this study is that the defect location is mainly confined to the foot dorsum. However, foot defects can occur in various anatomical locations on the foot, and since the foot dorsum and plantar have their own uniqueness, these factors can influence the choice of reconstruction method and prognosis. According to clinical anatomy study by Custozzo et al. [19], when viewed from the caudal side, the foot dorsum is composed of thin skin, dorsal superficial fatty layer, superficial fascia, dorsal intermediate fatty layer, dorsal deep fascia, dorsal deep fatty layer, and dorsal deep fascia. This uniquely layered structure contributes to elasticity and pliability of the foot dorsum. However, the epidermal thickness of glabrous skin, which can range from 10 mm to 13 mm, gives special potential for resistance and defense to the plantar side of the foot [20]. Strong dermal adhesion to the deep plantar fascia via fibrous septa arranged in a honeycomb pattern allows for sufficient load absorption and redistribution. It seems that more specific results can be obtained by dividing the defect locations by dorsum and plantar.
A previous study conducted in our institute compared the use of fascial free flap and fasciocutaneous free flap for reconstruction of hand dorsum defects and found that the fascial free flap achieved a contour that was 1.5 times thinner than that of the unaffected contralateral side [21]. As a result, the patients showed positive responses regarding aesthetic satisfaction. Although there was a limitation that there was no modality to compare thickness in this comparative study, the aesthetic satisfaction of the patients was also high in the fascial group. It is expected that fascial free flap can produce satisfactory results for patients when aesthetic satisfaction is an important consideration in both lower and upper extremities. Like the hand dorsum, the foot dorsum is also exposed to the outside when wearing shoes such as sandals and flip-flops, so these factors should be actively considered.
Dryness was a prominent complaint in patients who had undergone fascial free flap. Eczema and dryness are caused by the devitalization and disruption of sebaceous glands in harvested STSGs [22]. Additionally, this can impede the secondary wound of the recipient site from healing. Most patients with fascial free flap complained of discomfort, finding it difficult to wear shoes due to dryness. The degree of occurrence of dryness and the resulting discomfort were investigated. More problems occurred in the fascial group, and it appeared that there was a statistically significant correlation. However, on the other hand, aesthetic satisfaction was significantly higher in the fascial free flap group. It suggests that the aesthetic satisfaction is higher when the fascial free flap is implemented, but in practical daily life use, discomfort occurs when wearing shoes or walking due to dryness and less improved sensation. Therefore, it seems that which is better between aesthetic satisfaction and practical benefit should be decided through a conversation between the surgeon and the patient before surgery.
Many efforts have been made to reduce the necessity of secondary debulking surgery after ALT free flap. A technique such as thin ALT free flap, which involves performing defatting procedure at the same time as harvesting the ALT flap to obtain a thinner free flap, is also being used [23]. Intraoperative massive defatting procedure during flap elevation, as proposed by Kimura et al. [24], can potentially save time that would otherwise be used for a secondary debulking procedure, and result in a uniformly thin flap. However, this technique can increase the risk of partial flap loss by interrupting the microcirculation of the flap [25]. According to additional research, it has been reported that the complication rate of primary thinning is higher compared to secondary debulking [26]. In our study, the fascial free flap had certain advantages over the thin ALT free flap due to the fact that its pedicle is intact within the flap and the surgery does not involve a defatting procedure that could potentially affect circulation or lead to other complications. Therefore, we concluded that the combination of the fascial free flap and STSG included in our study has several advantages over the thin ALT free flap technique in these aspects.
Another limitation of this study is the relatively small number of patients in each group, which may have made it difficult to statistically compare the results. As the number of patients increases, further studies could be conducted to confirm these findings.
Foot reconstruction is a challenging issue for both surgeon and patient, as its clinical outcome significantly affects function and aesthetic satisfaction. After proper diagnosis between fasciocutaneous and fascial ALT free flaps in foot, our data suggest that each surgical option has its pros and cons. Patients with fasciocutaneous free flap may have a better functional outcome, while patients with fascial free flap present with the better aesthetic outcome. Therefore, the discretion of surgeon and patient’s preference are factors to consider for the particular flap chosen for foot reconstruction.
Fig. 1.
(A) A 36-year-old male patient sustained an injury to his left foot from a motor vehicle injury. Debridement and negative pressure wound therapy was applied, but tendons were exposed. (B) The defect was covered using an anterolateral thigh fascial free flap. (C) Postoperative photograph after flap insetting. (D) A split-thickness skin graft was performed after 4 weeks.
Written informed consent was obtained from the patient above for the publication of this report including all clinical images.

Fig. 2.
(A) A 68-year-old female patient sustained an injury to her right foot from a motor vehicle injury. (B) An anterolateral thigh fasciocutaneous flap was elevated. (C) Follow-up at postoperative follow-up. (D) Follow-up at postoperative 3 weeks.
Written informed consent was obtained from the patient above for the publication of this report including all clinical images.
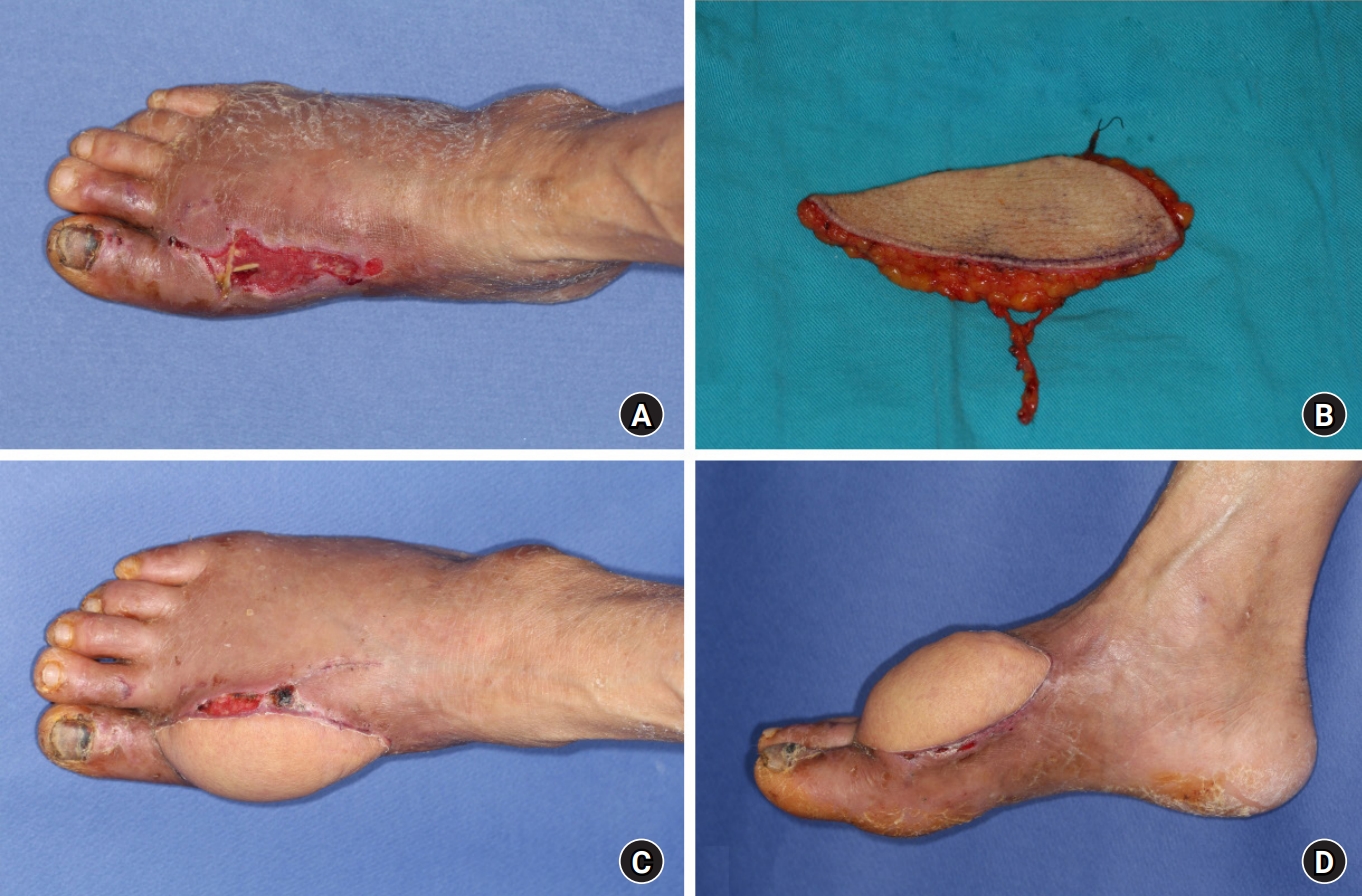
Table 1.
Postoperative dryness questionnaire
| Dryness | Severity |
|---|---|
| 0 | No difference between before and after the operation |
| 1 | Less severe |
| 2 | Slightly severe |
| 3 | Severe |
| 4 | Very severe |
| 5 | Extremely severe, affecting one’s daily living |
Table 2.
Postoperative discomfort due to dryness questionnaire
| Discomfort due to dryness | Severity |
|---|---|
| 0 | No discomfort at all |
| 1 | Less discomfort |
| 2 | Slight discomfort |
| 3 | More discomfort |
| 4 | Severe discomfort |
| 5 | Extremely severe discomfort that affects one’s daily living |
Table 3.
Aesthetic satisfaction questionnaire
Table 4.
Patients’ demographics and flap characteristics
Table 5.
Postoperative outcomes and sensory recovery outcomes
References
2. Song YG, Chen GZ, Song YL. The free thigh flap: a new free flap concept based on the septocutaneous artery. Br J Plast Surg. 1984;37:149-59.


3. Lee YC, Chiu HY, Shieh SJ. The clinical application of anterolateral thigh flap. Plast Surg Int. 2011;2011:127353.



4. Yang WG, Chiang YC, Wei FC, Feng GM, Chen KT. Thin anterolateral thigh perforator flap using a modified perforator microdissection technique and its clinical application for foot resurfacing. Plast Reconstr Surg. 2006;117:1004-8.


6. Hsieh CH, Yang CC, Kuo YR, Tsai HH, Jeng SF. Free anterolateral thigh adipofascial perforator flap. Plast Reconstr Surg. 2003;112:976-82.


7. Nasajpour H, Steele MH. Anterolateral thigh free flap for “head-to-toe” reconstruction. Ann Plast Surg. 2011;66:530-3.


8. Ozkan O, Coşkunfirat OK, Ozgentaş HE. The use of free anterolateral thigh flap for reconstructing soft tissue defects of the lower extremities. Ann Plast Surg. 2004;53:455-61.


9. Wei FC, Jain V, Celik N, Chen HC, Chuang DC, Lin CH. Have we found an ideal soft-tissue flap?: an experience with 672 anterolateral thigh flaps. Plast Reconstr Surg. 2002;109:2219-30.


10. Brenner P, Rammelt S, Gavlik JM, Zwipp H. Early soft tissue coverage after complex foot trauma. World J Surg. 2001;25:603-9.


11. Sato T, Yana Y, Ichioka S. Free flap reconstruction for diabetic foot limb salvage. J Plast Surg Hand Surg. 2017;51:399-404.


12. Kolbenschlag J, Hellmich S, Germann G, Megerle K. Free tissue transfer in patients with severe peripheral arterial disease: functional outcome in reconstruction of chronic lower extremity defects. J Reconstr Microsurg. 2013;29:607-14.


13. Lähteenmäki T, Waris T, Asko-Seljavaara S, Sundell B. Recovery of sensation in free flaps. Scand J Plast Reconstr Surg Hand Surg. 1989;23:217-22.


14. Lowrey CR, Strzalkowski ND, Bent LR. Skin sensory information from the dorsum of the foot and ankle is necessary for kinesthesia at the ankle joint. Neurosci Lett. 2010;485:6-10.


15. El-Gammal TA, El-Sayed A, Kotb MM, et al. Dorsal foot resurfacing using free anterolateral thigh (ALT) flap in children. Microsurgery. 2013;33:259-64.


16. Rhodius P, Haddad A, Matsumine H, et al. Noninvasive flap preconditioning by foam-mediated external suction improves the survival of fasciocutaneous axial-pattern flaps in a type 2 diabetic murine model. Plast Reconstr Surg. 2018;142:872e-883e.


17. Lee ZH, Abdou SA, Ramly EP, et al. Larger free flap size is associated with increased complications in lower extremity trauma reconstruction. Microsurgery. 2020;40:473-8.


18. Boca R, Kuo YR, Hsieh CH, Huang EY, Jeng SF. A reliable parameter for primary closure of the free anterolateral thigh flap donor site. Plast Reconstr Surg. 2010;126:1558-62.


19. Custozzo A, Frank K, Schenck TL, et al. Anatomy of the dorsum of the foot and its relevance for nonsurgical cosmetic procedures. Plast Reconstr Surg. 2020;146:64-72.


20. Sanchez BY, Gallardo DD, Espinoza JA, Soto DF. Subunit Principle: key element for plantar reconstruction with free sensate flaps. Arch Hand Microsurg. 2021;26:43-9.

21. Lee MG, Kim JS, Lee DC, Roh SY, Lee KJ, Choi BK. Fascial free flap for reconstruction of the dorsolateral hand and digits: the advantage of a thin contour. Arch Plast Surg. 2016;43:551-8.



22. Seyhan T. Split-thickness skin grafts. In: Marcia Spear, editor. Skin grafts: indications, applications and current research. Rijeka, Croatia: IntechOpen; 2011.
23. Kimura N, Satoh K. Consideration of a thin flap as an entity and clinical applications of the thin anterolateral thigh flap. Plast Reconstr Surg. 1996;97:985-92.


24. Kimura N, Satoh K, Hasumi T, Ostuka T. Clinical application of the free thin anterolateral thigh flap in 31 consecutive patients. Plast Reconstr Surg. 2001;108:1197-210.


-
METRICS

-
- 0 Crossref
- 981 View
- 53 Download
- Related articles in Arch Hand Microsurg
-
Usefulness of the lateral arm free flap for hand defect reconstruction2023 September;28(3)
Comparison of Bone Graft and Fixation Techniques in Scaphoid Nonunion2003 ;8(2)






