|
 |
- Search
| Arch Hand Microsurg > Volume 25(4); 2020 > Article |
|
Abstract
Snakebites, though uncommon, are a potentially serious cause of disability or death. Local symptoms may include pain, edema, or ecchymosis that may progress to skin necrosis or compartment syndrome. This study explores the case of a 4-year-old male patient bitten by a snake on the distal volar aspect of his left ring finger. On physical examination, there were moderate swelling, hemobullae formation, and the skin necrosis was progressing on middle phalanx of ring finger. Fasciotomy and topical oxygen therapy was performed. The topical oxygen therapy (TOT) was started once a day for 90 minutes with 4 L/minute of oxygen flow. TOT is a method of delivering humidified oxygen directly to the wound bed to support the healing of chronic and hypoxic wounds. There is no report on TOT for snakebite injury. In this report, we would like to report on the clinical experience of early surgery and adjuvant TOT with literary consideration.
Poisonous snake has specialized teeth which release venom from glands linked to the fangs. Skin necrosis at the bite site, to systemic symptoms including acute kidney injury, acute respiratory failure, acute myocardial infarction, disseminated intravascular, coma, coagulation, and death [1]. In a 2008 World Health Organization survey, about 421,000 people are bitten by snakes annually worldwide, of which 20,000 are killed. In South Korea, 192 to 621 people are bitten by snakes annually, and an average of 5 people are killed per year [2]. Especially in South Korea, distal parts of upper extremities are the most common sites of snakebite injuries [3]. Various severe complications in hands have been reported, including compartment syndrome, occasionally resulting in amputation. Given the importance of the functions of extremities, even localized symptoms of snakebites on extremities should be treated with the utmost care.
In the current study, we present a case of snakebite on the left ring finger, treated with surgical intervention and topical oxygen therapy (TOT) which has not been reported in previous studies. We believe this study will contribute to improved treatment of snakebite-induced soft tissue necrosis. The study was performed in accordance with the principles of the Declaration of Helsinki.
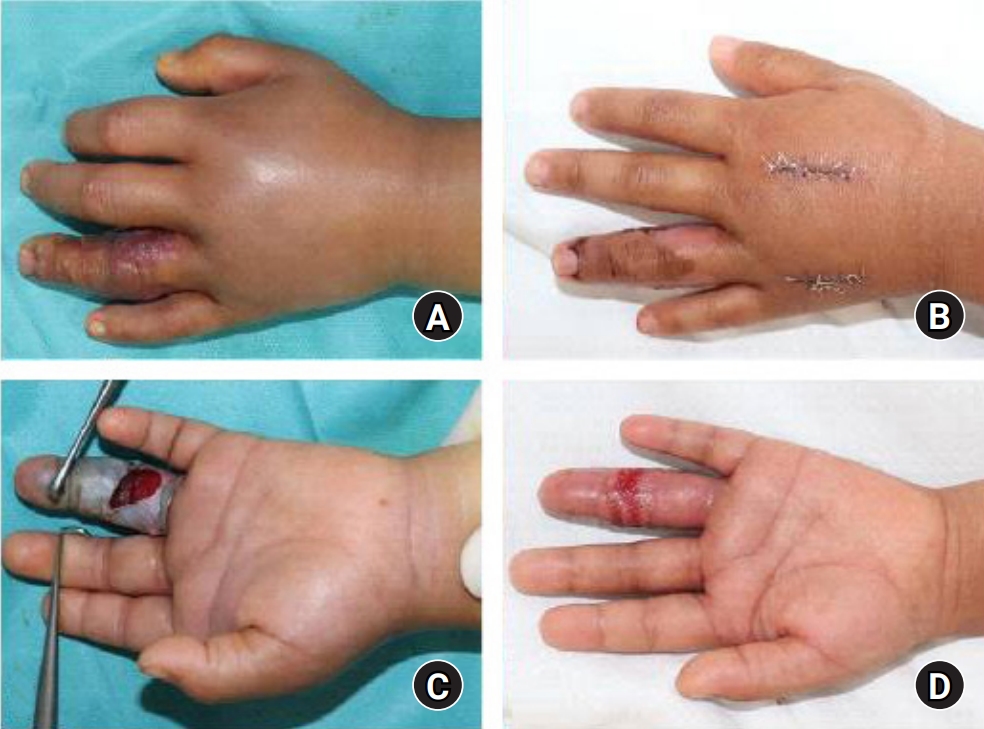
A 4-year-old boy who was healthy and never had undergone any disease was admitted with snakebite of his ring finger. He was bitten by a striped brown snake while going to the valley. After the injury, he was treated his finger by simple dressing with the laceration, empirical antibiotics, and antivenom at local clinic. After that, he transferred to our department for management on the same day. On physical examination, there were moderate tenderness, swelling, bullae formation, and skin necrosis that was progressing on the middle phalanx of ring finger (Fig. 1). But, there was neither exquisite tenderness along flexor tendon sheath nor marked pain on the proximal part of ring finger. Therefore, the possibility of tenosynovitis (TS) was low. On admission, he had a temperature of 37.3°C. Blood cultures, a full blood count, and a wound microbiology swab were taken and he was promptly commenced on intravenous cefaclor, analgesia, hand elevation, immobilization, and general bed rest. Radiologic inspection was carried out to confirm the presence of minute foreign body. There was no radiopaque densities seen as foreign body. The full blood count showed minor leukocytosis (14.4×109/L). There was no growth in wound cultures.
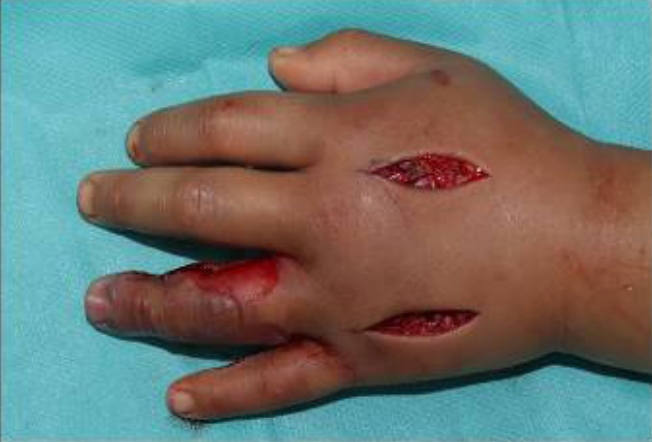
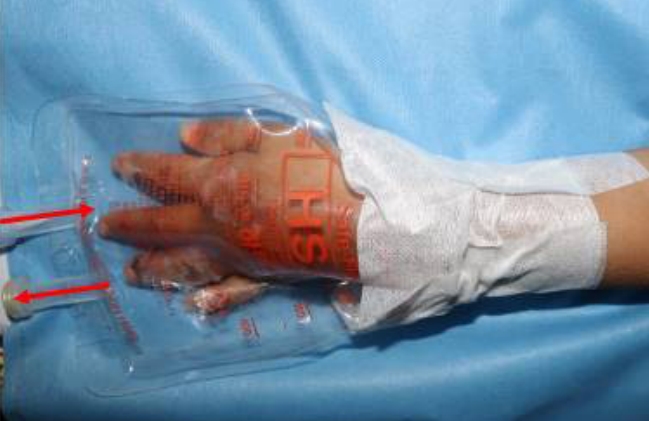
Although the treatment was maintained for 2 days with simple dressing and antivenom, his finger was exacerbated and seemed to be more swollen. So 3 days after the initial treatment, fasciotomy was performed on the hand dorsum and the ring finger for the lateral aspect, judging that the compartment syndrome could proceed due to the worsening of the swelling. Fasciotomy allowed oxygen to be supplied to deeper tissue. Also, negative pressure wound therapy was performed on the hand dorsum (Fig. 2). On the same day, TOT was started once a day for 90 minutes with 100% oxygen before daily dressing. After sealing the hand with an aseptic fluid pack, an O2 catheter was connected (Fig. 3). Antibiotic ointment was superficially applied on wound margin to prevent drying up. On TOT day 6%, 10%, 50%, and 80% epithelization was progressed respectively. TOT was carried out for a total of 12 days. He responded well to the treatment and was discharged after 19 days of hospitalization.
A total of 16 species of snakes are known to exist in Korea, of which only four are poisonous; three species of the genus Gloydius (G. brevicaudus, G. saxatilis, G. ussuriensis) and one species of the genus Rhabdophis (R. tigrinus) [4]. Studies so far have reported G. ussuriensis to be the predominant cause of snakebite due to its large population and easily accessible habitation area at the base of mountain or in farming area. There are no accurate statistics on the frequency of venomous snakebite injuries in Korea, although an average of 409.6 patients are reported to visit the hospital annually, which may increase when including patients with minor injuries who do not visit the hospital [5]. Patients with snakebite injuries develop a wide variety of clinical courses, from mild symptoms such as edema and pain at the injury site to serious complications including acute kidney injury, acute respiratory failure, acute myocardial hemoptysis, infarction, coma, disseminated intravascular coagulation, and death [1]. In our case, the patient had no systemic complication but had localized tenderness, swelling, and skin necrosis.
The hands especially the distal areas such as the fingers and palm, were the predominant sites of injury [3]. In this case, the patient was injured his left ring finger. Because hands, especially fingers, are one of the most important functional areas, so if not treated properly, it can cause serious side effects. In particular, the patient is not yet fully grown, which can lead to more fatal consequences [6].
In this case, we ruled out TS. But because snakebite injury is commonly accompanied by TS, physicians always should keep in mind the TS on patients with snakebite injury. TS initially starts with exudates within the tendon sheath leads to increased pressure, leading to ischemia. There are several signs which called Kanavel signs. There is tenderness along the sheath and finger sits in a resting flexed posture in patients with TS. Also, pain is more severe at the proximal part and fusiform swelling of the finger can be found. Treatment of TS involves broad-spectrum antibiotics and rapid surgery to debride tissues and irrigation [7].
Treatment of snakebite injury can be divided into surgical and nonsurgical treatment. From a surgical perspective, the first dilemma the clinician faces in managing a snakebite wound is determining whether to perform debridement on the wound site. In principle, trauma patients should undergo debridement as soon as possible, thereby removing the necrotized tissue in order to prevent further infection. In the past, early removal of snake venom by surgical methods was recommended as immediate management [6].
However, the majority of such treatments resulted in soft tissue damage, leading to failed skin graft or flap, amputation, and osteomyelitis, ultimately leading to a poor prognosis. Immediate debridement is no longer the treatment of choice in managing snakebites; rather, the current standard of care is administration of antivenom followed by delayed debridement. A recent study using an electron microscope observed viable tissues buried inside necrotized muscles of the snakebite wound, providing additional evidence for preemptive antivenom use followed by delayed debridement [6].
Oxygen therapy can be divided into hyperbaric oxygen therapy (HBOT) and TOT. As HBOT is systemic and raises the pressure of oxygen (pO2), there is a risk of complications such as seizures, damage to the tympanic membrane of the ear, and damage to the retinal nerve. If patients have diabetes, their glucose levels could also be affected by an increased pO2. Also, HBOT can only be performed in hospitals that have chamber and it is not cost-effective [8].
A study performed by Fries et al. [8] demonstrated that TOT promotes vascular endothelial growth factor expression in wound and neovascularization via pig models. Four female pathogen-free domestic pigs each had five wounds located on their backs, for a total of 20 wounds. Each wound consisted of a 2.5×2.5-cm excised full-thickness skin. Half of the wounds were treated with TOT using 100% oxygen at 1 atmosphere of pressure for 3 hours per day for the first 7 days of wounding; the other half of the wounds were treated with room air, dressed with a transparent dressing, and allowed to heal by secondary intention.
Studies have shown that TOT elevates tissue oxygen levels to a depth of 2 mm within the wound bed, stimulates neovascularization, supports synthesis and maturity of collagen deposition, leading to increased tensile strength and decreased recurrence of the wound [5]. Increased oxygen levels at the wound site have shown to lead to the timely closure of wounds. In this case, the patients had epidermal to dermal layer necrosis. And fasciotomy was performed, so oxygen could be supplied to the deep layer of wound sufficiently and may stimulate neovascularization and maturation of collagen deposition.
TOT is a noninvasive, portable therapy that uses a reusable acrylic chamber, vinyl extremity boot, or vinyl multipurpose bag to deliver oxygen directly to the wound bed. This method of delivery achieves tissue penetration and increased oxygen levels in the open wound without risk of systemic oxygen toxicity. TOT has merit that can be applied anytime, anywhere 24 hours a day in a cost-effective manner, and there is no risk such as systemic oxygen poisoning.
So far, there have been no reports of TOT for the snakebite injury. This case report is meaningful in that it showed the possibility that the TOT may be helpful in snakebite injury. When patients with snakebite visit, because TOT is cost-effective, noninvasive, and there are few complications, physicians can consider trying it as adjuvant therapy.
Acknowledgements
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (2020R1A2C1100891), and was supported by Soonchunhyang University research fund.
REFERENCES
2. Kasturiratne A, Wickremasinghe AR, de Silva N, et al. The global burden of snakebite: a literature analysis and modelling based on regional estimates of envenoming and deaths. PLoS Med. 2008;5:e218.



3. Shin CS, Bae JS, Sohn KS. Clinical analysis on venomous snake bite in Korea. J Korean Surg Soc. 1984;27:245-54.
4. Lee BJ, Hong SI, Kim HS, et al. Hematological features of coagulopathy and the efficacy of antivenin therapy for a Korean snakebite. J Korean Surg Soc. 2007;72:18-26.
5. Orsted HL, Poulson R; Advisory Group, et al. Evidence-based practice standards for the use of topical pressurised oxygen therapy. Int Wound J. 2012;9:271-84.



6. Rha JH, Kwon SM, Oh JR, Han BK, Lee KH, Kim JH. Snakebite in Korea: a guideline to primary surgical management. Yonsei Med J. 2015;56:1443-48.



-
METRICS

-
- 2 Crossref
- 3,601 View
- 73 Download
- Related articles in Arch Hand Microsurg
-
Treatment of Bony Mallet Finger with Extension Block Technique2005 December;10(4)
Treatment of Scaphoid Nonunion with Inlay Bone Graft2003 ;8(3)
Treatment of the Finger Flexion Contracture with Arterialized Venous Free Flap2004 October;13(2)