 |
 |
- Search
| Arch Hand Microsurg > Volume 25(3); 2020 > Article |
|
Abstract
Purpose
Intraoperative indocyanine green (ICG) lymphography is an effective tool to obtain real-time video images of functioning lymph vessels in edematous limbs. However, it is difficult to identify the course of lymph vessels in obese patients or patients with large dermal backflow. Without the image, surgeons have to rely on their experience when performing the skin incision to locate the lymphatic vessels. This study focused on elucidating lymphatic vessel flow patterns in healthy lower extremities in an Asian population to refer these findings for lymphedema treatment.
Methods
ICG fluorescence lymphography was performed by injecting 0.2 mL of ICG into the first web space of the foot. After 4 hours, fluorescence images of lymphatic vessels were obtained and the lymphatic vessels were marked. Three landmarks were designated; the medial malleolus, the medial patellar border, and the groin femoral artery. Straight lines connecting the points were drawn, and the distance between the connected lines and the marked lymphatic vessels was measured in eight points.
Results
Fifteen subjects with healthy lower extremities (15 right and 15 left) were included. The average course of the main lymph vessels passed 26.2±18.0 mm dorsally to the medial malleolus, 53.7±35.7 mm medially to the medial patellar border, and 25.5±19.2 mm medially to the three-quarters point of the upper landmark line.
Lymphedema is a disease due to the impairment of the lymphatic system. After suffering from the surgery, radiation therapy, infection, or trauma, patient’s lymphatic system can be disrupted and lead progressive fluid retention and tissue swelling [1]. Lately, lymphedema has been receiving more attention since it is a relatively common complication after the cancer treatment [2].
In lymphedema, structural changes in the lymphatic system precede clinical symptoms such as pain and change in appearance. The structural changes include abnormal lymphatic vessel dilation and twisting. Abnormal retention of contrast medium due to the change was reported in an imaging study as a result [3].
The conservative treatment of lymphedema includes compression garments, intensive bandaging, and massaging of the affected limb. For patients unresponsive to theses conservative therapies, surgical options are recommended. The options are circumferential liposuction, microsurgical lymphovenous shunts, and vascularized lymph node transfer [2]. Among various surgical options lymphovenous anastomosis (LVA), which connects functioning lymphatics with small vein, has several advantages over other procedures. It can be performed under local anesthesia, is less invasive compared to other surgical techniques, and is effective in severe cases that are refractory to conservative therapy [4-8]. To maximize the therapeutic effect of LVA, proper identification of the functioning lymphatic vessels and accurate incision for anastomosis within a limited operative time are important [4-9]. Lymphatic vessels undergo degeneration as lymphedema progresses, and it is difficult to find functioning lymph vessels in late-stage lymphedema. Surgical results of LVA are much favorable when functioning lymphatics are bypassed.
Indocyanine green (ICG) lymphography has lately been used to visualize the superficial lymphatic flow. ICG as a tracer for lymphography is a safe, effective, and minimally invasive method. Lymphatic vessel imaging allows surgeons to detect the precise location of the lymphatic vessels for microscopic surgery [1,8,10-13]. Near-infrared camera is used to obtain real-time video images by tracing ICG dye movement [14]. However, it is difficult to clearly identify the course of lymphatic vessels in obese patients and advanced lymphedema patients. As lymphedema progresses, dermal backflow makes it difficult to identify underlying lymphatic vessel course. Finding functioning lymphatics is not easy in patients with large dermal backflow [13]. In such cases, surgeons might have to rely on their experienced intuition to locate skin the incision for large functioning lymphatic vessels [15].
A previous cadaver study revealed that large lymphatic vessels in the lower extremity travel close to the saphenous vein of the leg [16]. The purpose of this study was to reveal the lymphatic vessel flow patterns in healthy lower extremities and to propose a reference for the lymphedema treatment.
This study protocol was approved by the Institutional Review Board of Korea University Ansan Hospital (No. AS17191). All volunteers provided written informed consent for participation in this study and the publication of their clinical images.
Between March 2016 and July 2017, we conducted a study using ICG lymphography. Fifteen volunteers (13 males, 2 females) were included in this study. Overall, 30 lower extremities were evaluated (bilateral limbs of 15 healthy volunteers). The age of the volunteers ranged between 24 and 46 years (mean, 29.0 years), and body mass index ranged between 20.4 and 27.1 kg/m2 (mean, 23.2 kg/m2) (Table 1).
Subcutaneous injection of 0.2 mL of ICG (Dongindang Pharm. Corp. Ltd., Siheung, Korea) was injected into the lower extremities at the first web space of the foot. After 4 hours, fluorescence images of the lymphatic vessels were obtained with a near-infrared camera (Moment K; IAN C&S, Seoul, Korea), and the lymphatic vessels were marked (Figs. 1, 2). Three landmarks were designated as (1) the medial malleolus, (2) the medial patellar border, and (3) the groin femoral artery. A straight line connecting the points was drawn, and the distance between the connected lines and the marked lymphatic vessels was measured in eight points (Fig. 3). If two or more lymph vessels were visible, the one with the largest diameter was chosen. If they appeared similar, the middle position was marked. All data were expressed as means and standard deviations (Fig. 4).
Fifteen subjects with healthy lower extremities (15 left and 15 right) were included in this study. From the distal end, the lymphatic vessels ran dorsally to the medial malleolus, passed posteriorly to the medial patellar border, and then coursed toward the inguinal lymph nodes (Fig. 2). The average course of the main lymph vessels passed 26.2±18.0 mm dorsally to the medial malleolus, 53.7±35.7 mm medially to the medial patellar border, and 25.5±19.2 mm medially to the three-quarters point of the upper landmark line (Fig. 4). Also, the ratio of the distance between the marked lymphatic vessels and landmarks to the circumference of each point was calculated and expressed in percentages (Table 2, Fig. 4)
Lower extremity lymphedema is a stressful complication that can occur after the treatment of cancers, including breast cancers, gynecologic cancers, and urologic cancers [2]. It frequently goes through a chronic course and is difficult to manage [17]. Among several diagnostic tools for examining lymphedema, lymphoscintigraphy is widely used to detect abnormal lymphatic circulation and to localize the lymph nodes. However, its drawback is that it involves radiation exposure due to the use of a radioisotope and cannot visualize the precise course of the lymphatic vessels [13].
On the other hand, ICG lymphography uses a non-radioactive medium as a tracer. Since it does not carry a potential risk of radiation, ICG lymphography is widely used for evaluating lymphedema [1,10,12,14,18-20]. In 2007, Ogata et al. [1] and Unno et al. [19] reported the clinical application of ICG lymphography for the evaluation of lymphedema. Many authors investigated the clinical applications of ICG lymphography and obtained important information for lymphatic functional assessment and preoperative evaluation before microsurgical procedures [1,10,14,19]. The sensitivity of lymphedema detection using ICG lymphography was almost 100% in a rat model [1]. With a proper injection of ICG into a subcutaneous layer devoid of blood vessels, the medium flows into the lymphatic system. Even though ICG is mistakenly injected into an artery or a vein, the blood flow washed the medium away in less than a minute. Therefore, accidentally injected medium did not affect the overall results [1].
Conservative and surgical treatment options for lymphedema are available. Most early-stage patients choose conservative treatment options using various compression therapies such as complex physical therapy, pneumatic pumps, and compressive garments [2,21]. After distressful conservative treatment fails, surgery is considered [8]. Various surgical methods are under practice including LVA, vascularized lymph node transfer, and suction-assisted lipectomy. Among these surgical treatments, LVA, which involves a bypass connecting the congested lymph vessels to the venous system, is the least invasive and most effective surgical treatment [8].
Many surgeons employed ICG lymphography to visualize the superficial lymphatic flow. Since it allows real-time visualization of superficial (1 to 2 cm in depth) lymphatic vessels, the surgeons can identify the exact location of lymphatic vessels for LVA surgery [1,8,10-13]. Acquired information allows surgeons to more accurately determine the skin incision site for LVA, to shorten the incision length, and to reduce the operative time [6,8].
However, ICG lymphography also has a limitation. It is hard to locate the lymphatic vessels deeper than 2 cm from the skin. Moreover, the technology is less accurate in advanced stage cases with the extension of dermal backflow (DB) patterns [11-13]. Unfortunately, large DB patterns frequently exist in patients with clinically early-stage lymphedema cases obscuring the lymphatic vessel visualization [8]. The limited image makes surgeons difficult to determine the incision site for LVA. To unburden such difficulty, we identified the approximate location of the lymphatic vessels in the lower extremities of healthy persons for use as a reference during surgery.
In 2016, Amore et al. [16] reported that the course of superficial lymphatic vessels was often concentrated near the superficial venous system, especially the saphenous veins. According to that study, lymph vessels from the foot and the leg flowed into the lymph nodes of the inguinal region, which is consistent with our findings.
This study has some limitations. First, only 30 lower extremities are relatively small study groups. Second, the research group included only Asian volunteers. Third, more male volunteers than female volunteers were included due to some hesitation regarding body exposure. Fourth, the detection depth of the infrared camera system was limited and only the lymph vessels located in the dermis and subcutaneous fat layer were determined. The deep lymphatic system could not be assessed. The superficial lymphatics in patients with early-stage of lymphedema are usually maintained and might be more important for the operation than the deep lymphatic chains [14]. Fifth, only large lymphatic collectors were traced. The diameter of lymphatic vessel is crucial for LVA and use of large functioning lymph vessel allows small number of anastomosis for clinical improvements. Recent studies on LVA have shown that lymphatic vessels between 0.3 and 0.6 mm in diameter are used in the surgery [6]. For example, in the study by Yamamoto et al. [8], LVA was successfully performed in a 0.45-mm-diameter lymphatic vessel.
The significance of our study was that to the best of our knowledge it was the first to demonstrate and quantify the location of functioning lymphatic vessels in the lower extremities of a healthy Asian population. In our study, the distance between the lymphatic vessel and the landmark was divided by circumference and expressed as a percentage to account for physical differences among the subjects. In this way, it can help surgeons locate incisions in difficult situations.
Fig. 1.
A real-time indocyanine green (ICG) fluorescence image. An ICG fluorescence image was taken with a near-infrared camera four hours after injection of ICG dye. Lower extremity lymphatic flow can be clearly detected. The arrow indicates the knee.
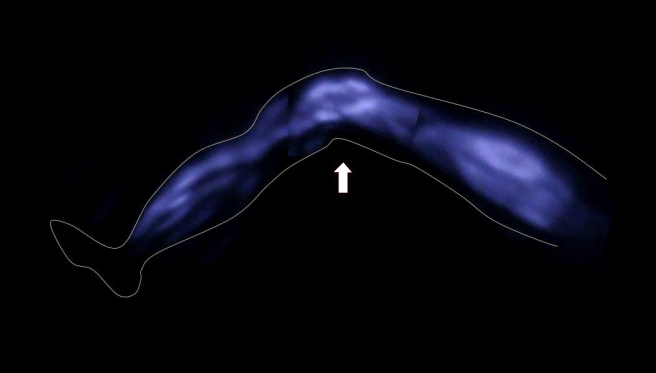
Fig. 2.
Lymphatic vessels are marked on the body. Each small ‘×’ represents a landmark, and the purple line indicates lymphatic vessels detected with a near-infrared camera.
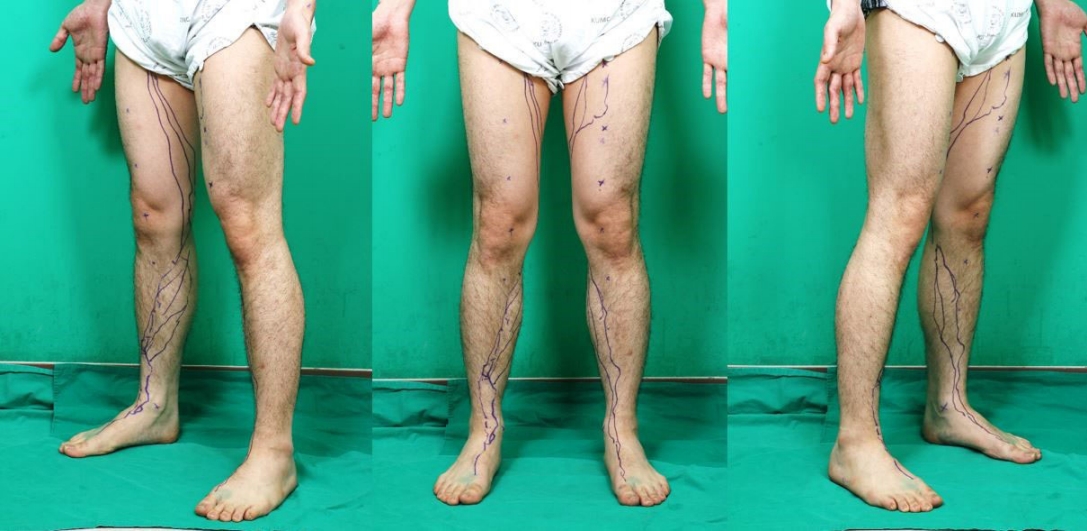
Fig. 3.
An illustration of the landmarks. A straight line connecting the points that were drawn and divided into four equal lengths.
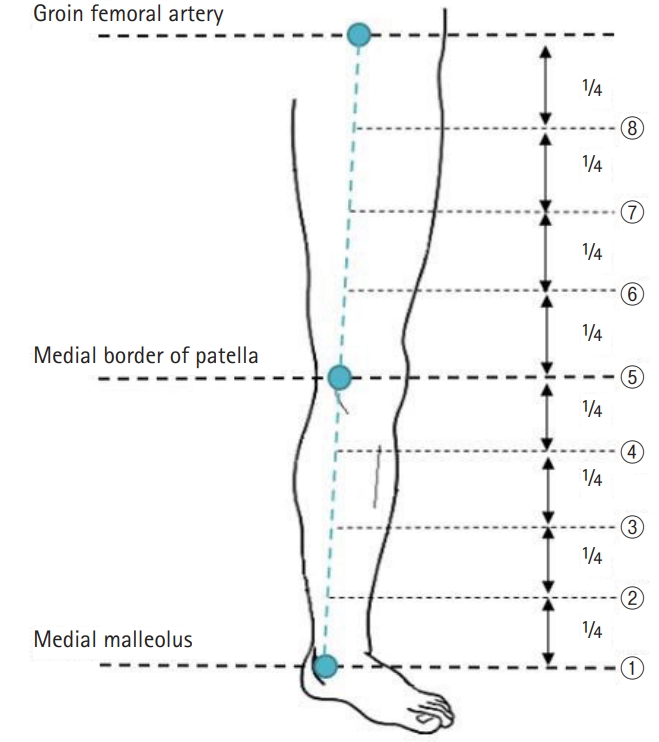
Fig. 4.
Lymphatic vessel courses in healthy volunteers. The distance between the connecting line and the marked lymphatic vessels was measured. In addition, the distance from each landmark to the lymphatic vessel (mean±standard deviation) was divided by the circumference and calculated as a percentage. Positive values mean anterolateral position of lymphatic vessels relative to landmarks. Negative values mean posteromedial position of lymphatic vessels.

Table 1.
Characteristics of 30 participants with healthy lower extremities
| Characteristic | Mean ±SD (range) |
|---|---|
| Age (yr) | 29.0±6.4 (24–46) |
| Height (cm) | 173.7±7.2 (158–188) |
| Weight (kg) | 70.1±8.7 (56–84) |
| Body mass index (kg/m2) | 23.2±1.9 (20.4–27.1) |
Table 2.
Course of lymphatic vessels in healthy volunteers
| Landmark | Mean distance (mm) | Relative distance (%)a) |
|---|---|---|
| Groin femoral artery (A) | - | - |
| 3/4 point between A and B | –25.5±19.2 | –4.7±3.3 |
| 2/4 point between A and B | –45.2±24.6 | –9.0±4.7 |
| 1/4 point between A and B | –58.0±32.8 | –13.2±7.2 |
| Medial border of patella (B) | –53.7±35.7 | –14.6±9.2 |
| 3/4 point between B and C | –22.9±24.2 | –6.5±6.8 |
| 2/4 point between B and C | –10.2±28.3 | –2.9±7.9 |
| 1/4 point between B and C | 10.7±18.2 | 4.4±7.5 |
| Medial malleolus (C) | 26.2±18.0 | 11.0±7.9 |
REFERENCES
1. Ogata F, Azuma R, Kikuchi M, Koshima I, Morimoto Y. Novel lymphography using indocyanine green dye for near-infrared fluorescence labeling. Ann Plast Surg. 2007;58:652-5.


2. Warren AG, Brorson H, Borud LJ, Slavin SA. Lymphedema: a comprehensive review. Ann Plast Surg. 2007;59:464-72.


4. Yamamoto T, Narushima M, Kikuchi K, et al. Lambda-shaped anastomosis with intravascular stenting method for safe and effective lymphaticovenular anastomosis. Plast Reconstr Surg. 2011;127:1987-92.


5. Campisi C, Boccardo F. Microsurgical techniques for lymphedema treatment: derivative lymphatic-venous microsurgery. World J Surg. 2004;28:609-13.


6. Koshima I, Inagawa K, Urushibara K, Moriguchi T. Supermicrosurgical lymphaticovenular anastomosis for the treatment of lymphedema in the upper extremities. J Reconstr Microsurg. 2000;16:437-42.


7. Koshima I, Nanba Y, Tsutsui T, Takahashi Y, Itoh S. Long-term follow-up after lymphaticovenular anastomosis for lymphedema in the leg. J Reconstr Microsurg. 2003;19:209-15.


8. Yamamoto T, Narushima M, Yoshimatsu H, et al. Minimally invasive lymphatic supermicrosurgery (MILS): indocyanine green lymphography-guided simultaneous multisite lymphaticovenular anastomoses via millimeter skin incisions. Ann Plast Surg. 2014;72:67-70.


9. Yamamoto T, Koshima I, Yoshimatsu H, Narushima M, Miahara M, Iida T. Simultaneous multi-site lymphaticovenular anastomoses for primary lower extremity and genital lymphoedema complicated with severe lymphorrhea. J Plast Reconstr Aesthet Surg. 2011;64:812-5.


10. Ogata F, Narushima M, Mihara M, Azuma R, Morimoto Y, Koshima I. Intraoperative lymphography using indocyanine green dye for near-infrared fluorescence labeling in lymphedema. Ann Plast Surg. 2007;59:180-4.


11. Yamamoto T, Matsuda N, Doi K, et al. The earliest finding of indocyanine green lymphography in asymptomatic limbs of lower extremity lymphedema patients secondary to cancer treatment: the modified dermal backflow stage and concept of subclinical lymphedema. Plast Reconstr Surg. 2011;128:314e-321e.


12. Yamamoto T, Narushima M, Doi K, et al. Characteristic indocyanine green lymphography findings in lower extremity lymphedema: the generation of a novel lymphedema severity staging system using dermal backflow patterns. Plast Reconstr Surg. 2011;127:1979-86.


13. Yamamoto T, Yamamoto N, Doi K, et al. Indocyanine green-enhanced lymphography for upper extremity lymphedema: a novel severity staging system using dermal backflow patterns. Plast Reconstr Surg. 2011;128:941-7.


14. Unno N, Nishiyama M, Suzuki M, et al. Quantitative lymph imaging for assessment of lymph function using indocyanine green fluorescence lymphography. Eur J Vasc Endovasc Surg. 2008;36:230-6.


15. Seki Y, Yamamoto T, Yoshimatsu H, et al. The superior-edge-of-the-knee incision method in lymphaticovenular anastomosis for lower extremity lymphedema. Plast Reconstr Surg. 2015;136:665e-675e.


16. Amore M, Tapia L, Mercado D, Pattarone G, Ciucci J. Lymphedema: a general outline of its anatomical base. J Reconstr Microsurg. 2016;32:2-9.


17. Shah C, Vicini FA. Breast cancer-related arm lymphedema: incidence rates, diagnostic techniques, optimal management and risk reduction strategies. Int J Radiat Oncol Biol Phys. 2011;81:907-14.


18. Tomczak H, Nyka W, Lass P. Lymphoedema: lymphoscintigraphy versus other diagnostic techniques: a clinician’s point of view. Nucl Med Rev Cent East Eur. 2005;8:37-43.

19. Unno N, Inuzuka K, Suzuki M, et al. Preliminary experience with a novel fluorescence lymphography using indocyanine green in patients with secondary lymphedema. J Vasc Surg. 2007;45:1016-21.


20. Unno N, Nishiyama M, Suzuki M, et al. A novel method of measuring human lymphatic pumping using indocyanine green fluorescence lymphography. J Vasc Surg. 2010;52:946-52.


-
METRICS

-
- 2 Crossref
- 3,390 View
- 63 Download
- Related articles in Arch Hand Microsurg
-
Lymphaticovenous Anastomosis in Lower Extremity Lymphedema: A Case Report2018 June;23(2)






