|
 |
- Search
| Arch Hand Microsurg > Volume 25(2); 2020 > Article |
|
Abstract
As deep inferior epigastric artery perforator (DIEP) flap surgery is gaining popularity, more patients including BRCA-positive patients need simultaneous laparoscopic surgery. We share our experience on a patient who underwent concurrent laparoscopic hysterectomy during flap elevation with a novel method. A patient diagnosed with a right breast cancer also required laparoscopic hysterectomy due to multiple uterine myoma. After perforator mapping was performed, flap elevation through external oblique fascia level was carried out first, sparing the periumbilical perforator and superficial inferior epigastric vein. Three ports were inserted for laparoscopy on posterior fascia level in the periumbilical area, left upper quadrant area and suprapubic area. The surgery was completed without any complication, gas leaks or vascular injury with the advantage of reduced risk of vascular damage and less surgical incision.
Deep inferior epigastric artery perforator (DIEP) flap surgery is one of the gold standards of immediate breast reconstruction. As DIEP flap gains its popularity, there are cases requiring both DIEP flap and laparoscopic surgery. As laparoscopic surgeries and abdomen-based flap surgeries share the field and put the patient at risk of vascular damage, there is a need to standardize multidisciplinary strategy before the operation. The purpose of this report is to introduce our novel method of placing ports for laparoscopy and to share our experience in such cases.
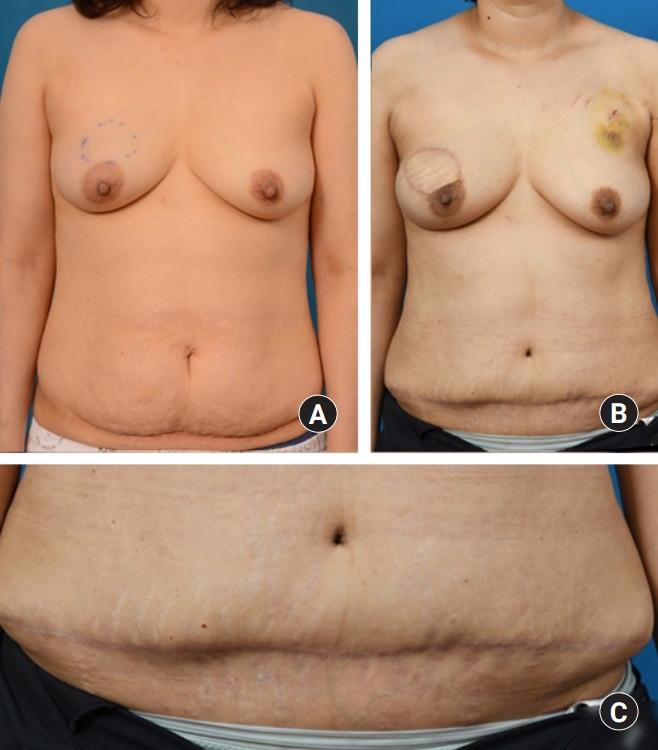
A 45-year-old female patient, initially complained of a palpable mass in the right side of her breast, was diagnosed malignant spindle cell tumor which needed wide excision of skin on the superolateral side of the nipple. Supported by the patient’s own preference for autologous reconstruction, DIEP flap was selected. The patient underwent preoperative computed tomographic (CT) angiography and hand held Doppler analysis for mapping perforators. During evaluation, multiple uterine myoma with cystic change and secondary degeneration was found (Fig. 1). This condition required concurrent total hysterectomy and possible bilateral salpingo-oophorectomy with laparoscopy.
Elevation of flap was planned to use a left side contralateral perforator which was 6 cm from the umbilicus (Fig. 1), while hysterectomy required transvaginal maneuver and 3 port routes—one periumbilical main port for endoscope and gas inflation, a second port in the left quadrant area, and third one in the suprapubic area. Informed consent was obtained from the patient for all specialties prior to surgery.
In the lithotomy position, an incision was made along the upper part of DIEP flap design and umbilicus. With adequate beveling of subcutaneous fat, dissection through the external oblique fascia was performed. A sufficient area near the umbilicus was dissected to allow initial trocar puncture, then an incision along the lower border of the flap design was also made, followed by avoiding injury to the superficial inferior epigastric vein (SIEV) (Fig. 2). The gynecologic team stepped in for placement of the initial trocar in the periumbilical linea alba. A second and third port were also successfully placed on the level of the fascia.
Hysterectomy with salpingo-oophorectomy was performed without any unexpected events and with proper pneumoperitoneum. Thirty-five minutes of dissection was needed before trocar insertion, and it took 125 minutes to finish laparoscopic surgery. All of posterior fascia was closed, and the skin was sutured with a temporary stapler and Ioban drape (3M Corporate, St. Paul, MN, USA) was applied. The patient was repositioned and redraped. No perforator nor SIEV injury was observed during DIEP flap elevation.
The concurrent breast reconstruction and mastectomy with laparoscopic surgery was successfully completed and the patient discharged from hospital without any wounds or laparoscopy related complication. No additional postoperative care was needed and no other events or complications related to the surgery were noted after 6 months of follow-up in an outpatient clinic (Fig. 3).
Some patients encounter the choice of whether to have concurrent laparoscopic surgery with DIEP flap. BRCA gene positive patients receiving prophylactic oophorectomy are typical candidates. Some clinics would rather separate the procedures but there have been studies that show the possibilities of combined procedure despite of structural difficulties of a multidisciplinary approach [1,2]. In some cases, surgery cannot be delayed for long because of the patient’s emergent condition.
As abdomen-based flap surgery directly shares its surgical field with laparoscopic surgeries, the possibility of vascular injury has been outlined by several studies [2,3]. Flap perforators lie around the periumbilical area which is close to port. SIEV, which can be used in the supercharging flap, is also prone to damage. These injuries are most likely to occur during trocar insertion, but can also take place when the ports are pulled strenuously during surgery. However, most articles focus on the methods of laparoscopy after abdomen-based flap surgery.
There are few reports about concurrent surgery and abdomen-based flap procedures. Spear et al. [1] mentioned in an article that an oophorectomy can simultaneously done via direct incision through the external oblique fascia, as an open technique without laparoscopy. Hunsinger et al. [2] described 8 cases of simultaneous laparoscopic oophorectomy with mastectomy and bilateral DIEP flap breast reconstruction in BRCA-positive patients. The authors place an initial port above the umbilicus to preserve perforator and lateral ports in an abdominoplasty scar. Therefore the method inevitably restricts original laparoscopic port location.
The novel approach presented above has several advantages over the previous one. Because trocars are inserted after direct visualization of perforator vessel of flap above fascia level, the method definitely obviates the possibility of injury to the perforators and protect them from traction injury. Main pedicle, deep inferior epigastric artery, is also preserved easily as its location becomes more apparent. Moreover, there is no additional scarring on the upper abdominoplasty flap or DIEP flap. Otherwise, the injury of upper abdominal flap may lead to donor site dehiscence or necrosis. Also, as the safety of vasculature and the scar issue is guaranteed, it is possible to modify port placement to wherever surgeons feel comfortable for laparoscopic surgery, except a region where rectus muscle and main artery lies under external oblique fascia. If laparoscopic team closes fascia before elevation of flap, there is also a possibility of tearing the site during the elevation of the DIEP flap, which can be prevented in the novel method (Fig. 1).
More cases are needed to establish the eligibility of the approach and to compare operation times or complications. Nonetheless, it could be uncomfortable for laparoscopic surgeons performing abdominal surgery because ports on the fascia could be unusual for them. A temporary skin stapler could alleviate this problem. Concerns over structural limitations due to the discomfort caused by involving multiple teams may be voiced in clinical practice but standardizing protocol will help to overcome such impediments.
In conclusion, simultaneous laparoscopic surgery can be successfully performed during DIEP flap elevation through the external oblique fascia. This method carries the advantage of a reduced risk of vascular damage and less surgical incision needed.
Fig. 1.
Computed tomographic angiography of the patient. (A) Perforator mapping for deep inferior epigastric artery perforator flap. (B) Multiple uterine myoma with secondary degeneration.
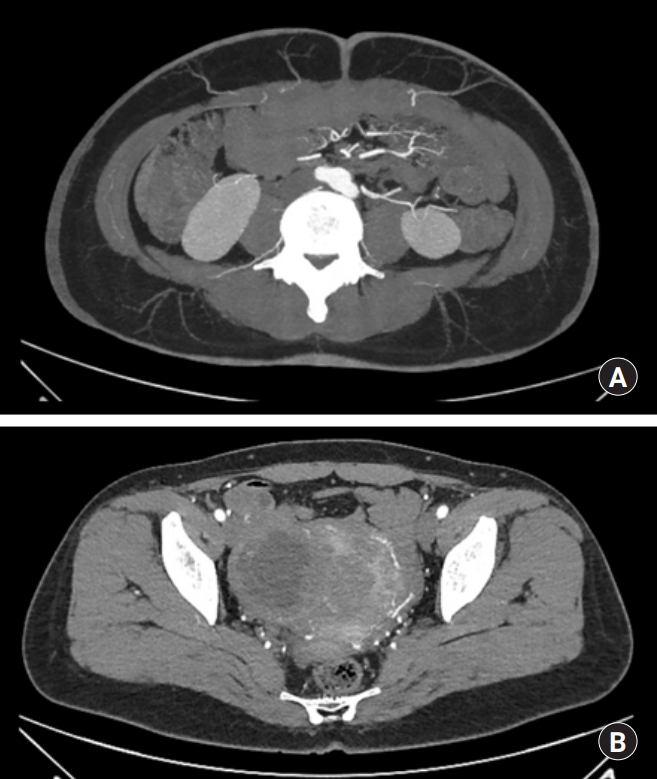
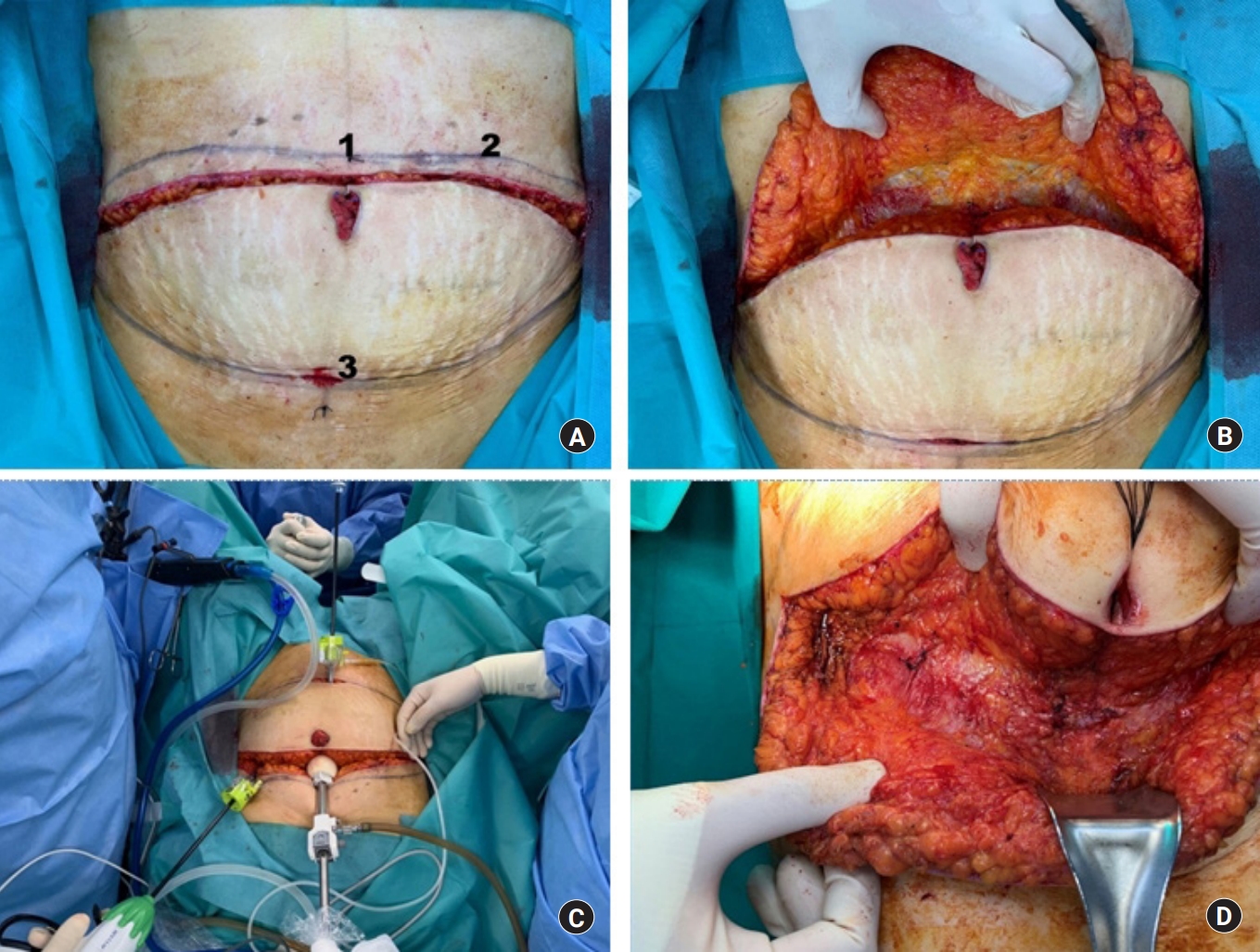
Fig. 2.
(A) Port placement plan after dissection through external oblique fascia (1, main port for endoscopy; 2, left upper quadrant port; 3, suprapubic port). (B) Dissection until external oblique fascia is reached. (C) Simultaneous laparoscopic surgery after port insertion. (D) Appropriate fascial closure after laparoscopic surgery.
REFERENCES
1. Spear SL, Pennanen M, Barter J, Burke JB. Prophylactic mastectomy, oophorectomy, hysterectomy, and immediate transverse rectus abdominis muscle flap breast reconstruction in a BRCA-2-positive patient. Plast Reconstr Surg. 1999;103:548-53.


-
METRICS

-
- 0 Crossref
- 3,422 View
- 49 Download
- Related articles in Arch Hand Microsurg
-
Topography of Deep Inferior Epigastric Perforator Flap2002 November;11(2)